Where you live may determine how you die
People along the southern stretch of the Mississippi River are more likely to die from heart problems than anywhere else in the United States.
Suicide and homicide will claim the most lives in the southwestern part of the country.
Deaths from chronic respiratory diseases are greatest in eastern Kentucky and western West Virginia.
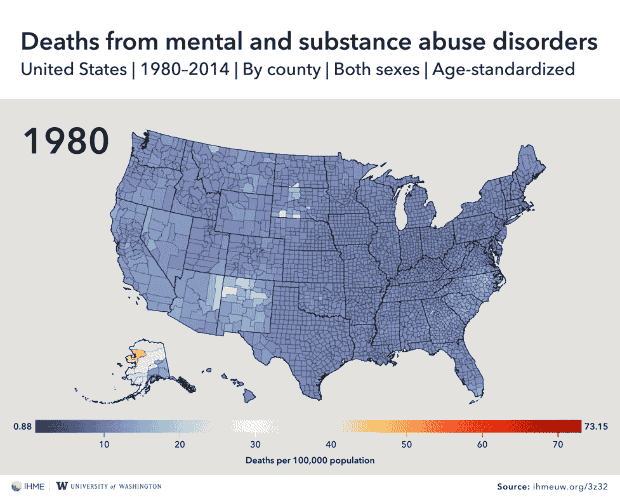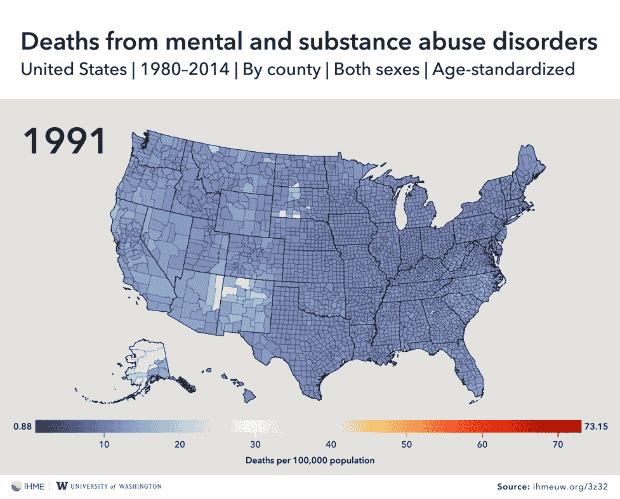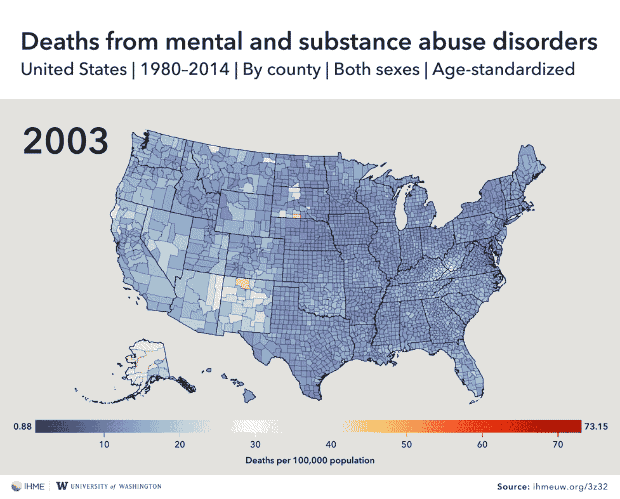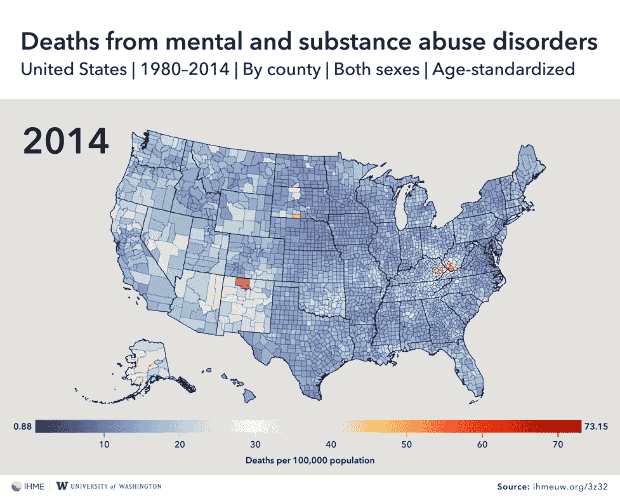
And mental and substance abuse disorders cause the most deaths in Alaska, eastern Arizona, New Mexico, eastern Kentucky and southwestern West Virginia.
What causes a person’s death depends in large part on where they spend their lives, concludes a new county-level analysis of U.S. mortality data.
Armed with this sort of information, county and city health departments can focus their efforts on the specific problems affecting their communities, said lead researcher Ali Mokdad. He is a professor with the department of global health at the University of Washington, in Seattle.
“You can see what kind of disparities we have, and what are driving these disparities,” Mokdad said. “Many counties, especially rural counties, don’t have the resources to tackle every health problem, and so they need to prioritize. In this way, we’re telling them what to tackle first.”
For the study, researchers reviewed more than 80.4 million deaths recorded from 1980 through 2014 in the United States, analyzing mortality rates for 3,110 counties or groups of counties.
The investigators found large disparities between counties for every cause of death, both within states and across the country as a whole.
For example, the researchers found that people in the southeastern United States are burdened with risk factors like obesity and smoking that increase the risk of dying from heart disease and diabetes, Mokdad said.
At the same time, people living in parts of New Mexico, Texas, Arizona, Nevada, Colorado, and North and South Dakota tend to drink more alcohol, and are more likely to die from cirrhosis or other chronic liver diseases, the findings showed.
On the other hand, people in northern and central Colorado benefit from “living healthier than anywhere else,” Mokdad said. “You see less death from certain chronic diseases. It’s clear that certain counties are in many ways less behind than the rest of the nation.”
There are four issues that mainly impact what researchers see in county-level death trends, Mokdad said:
- Social and economic factors, where poorer communities are less likely to live healthy.
- Access to health care, with some counties having many more uninsured people.
- Quality of health care, where doctors and patients are less likely to work together and follow up on control of risk factors, such as blood pressure or cholesterol.
- Preventable risky behaviors, including smoking, eating a poor diet, lack of physical activity and use of alcohol or drugs.
“The take-home from this study is that place matters,” said Dr. LaMar Hasbrouck, executive director of the National Association of County and City Health Officials.
“Place is the still the most important determinant of health,” Hasbrouck continued. “We need to zoom down to the granular level and look at the things that help drive health outcomes. Counties are going to have to do their own assessment to see what we’re missing here, and what resources we have to confront these issues.”
Mokdad hopes the new study will help counties get funding to confront their particular health dilemmas.
“Not only do they know what they have, but if they seek funding they can say this is our burden, this is how big the problem is, and we need money for it,” he said.
The county-level data also can help drive home specific health problems in communities where residents might be in denial, Mokdad added.
“If you come and say in the state of Washington smoking is high, then people in Seattle will say that’s not my problem, it’s happening elsewhere in the state,” he said. “But if you show it’s happening in Seattle, then people will see it’s their problem, it’s their burden and they have to deal with it.”
The study was published Dec. 13 in the Journal of the American Medical Association.