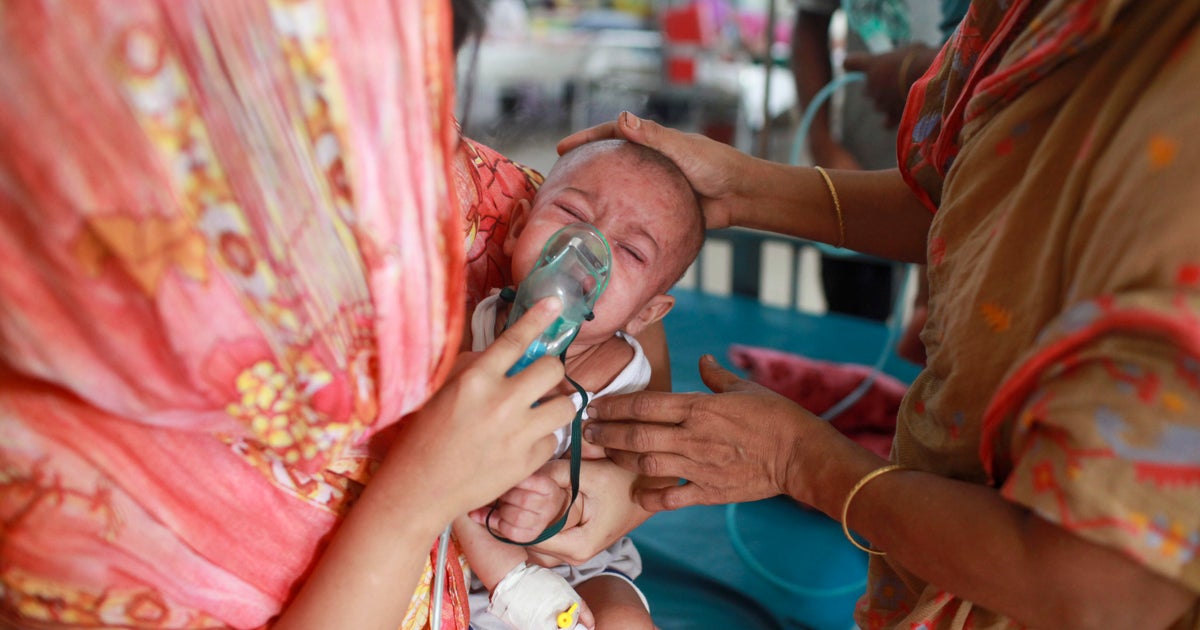
"We are not ready": Experts warn world is unprepared for next Ebola-size outbreak
Is the world ready to defend against the next big infectious disease outbreak? It’s one of the biggest threats humanity could face. But experts who have reviewed reports on the global response to the massive Ebola outbreak that swept through West African countries for two years starting in 2014 say we’re “grossly underprepared” to handle a similar health crisis.
A team headed by Dr. Suerie Moon, director of research at the Global Health Centre at the Graduate Institute of International and Development Studies in Geneva, published their findings from a review of seven major post-Ebola reports in the medical journal The BMJ at the end of January. The team concluded that, while progress has clearly been made by the world’s governments and the World Health Organization (WHO), for instance, there are gaps that could still leave millions of people at risk.
“I would say the biggest surprise from our findings was that there are some areas where there has been nothing done. There is a lot of agreement among the various reports, and certainly the reports focused on different aspects of what went wrong between lots of people from lots of organizations,” Moon told CBS News. “While there is a lot of agreement, there are certain areas that have been neglected.”
The research team’s findings cited a wide range of “neglected” areas, from the organizational failings at WHO to the ways in which other countries respond when news of an Ebola-type outbreak hits international media. For instance, Moon cited trade and travel restrictions that are often imposed when an outbreak is declared, often to the detriment of the affected country. The natural reaction is often “overreacted panic,” she said, spurring nations to “[put] in place a number of restrictions that don’t make sense.”
This kind of panic can have “huge repercussions in countries where the outbreak has been detected.” It can make leaders less willing to share information in the first place, a reaction fueled by fears over the economic consequences of disclosing the problem. And that silence can be dangerous — allowing an outbreak to fester and spread.
“A wakeup call”
In January 2016, WHO declared that the deadliest Ebola outbreak in history had come to an end, though it warned it would take several months before the world could be deemed conclusively free from the disease. The outbreak had claimed more than 11,300 lives since the first cases were detected in Guinea in March 2014.
The vast majority of the deaths happened in Guinea and its neighbors Liberia and Sierra Leone — but in our age of easy global air travel, no corner of the world was immune.
The first American case sparked panic nationwide and a number of drastic measures including quarantines to try to contain the threat.
Moon said the experience points out how important it is for the U.S. to work with other countries on this issue.
“International collaboration is an important pillar for protecting the health of Americans,” she said. “It’s not only about giving money — there really is an important self-interest rationale here in that this can impact Americans’ health.”
She urged the new administration to pay attention to the lessons of the past in preparing for the future.
“It’s crucial that the U.S. government and other countries of the world don’t forget about these countries several years after the outbreak hits its peak. There is a real risk that comes from people forgetting. It’s important to issue a wakeup call to policy makers — for instance, in the United States you have a new president who never dealt with Ebola in office before, so it’s important to remind him and his advisors that there is a lot that remains to be addressed.”
Another huge flaw Moon and her team pinpointed in their report was the fact that there is no “monitoring mechanism” in place to track various groups’ responses to outbreaks. Without a “centralized public information source,” she said, people will remain more vulnerable when future outbreaks hit.
“We need people to invest in monitoring what is happening — we have no good accountability in place,” she added. “You end up having to do a lot of detective work to examine what has been done and what is being done, and it shouldn’t be that hard.”
Moon also noted that the worst-hit countries are often those left very poor after years of internal conflicts. With few resources and weak public health systems, they are highly susceptible to outbreaks spreading out of control. Yet WHO finds itself in a difficult position, as an agency within the United Nations, “hesitant to take on some challenging political decisions that might upset leaders in these countries,” Moon suggested.
While things have improved — WHO’s response to last year’s Zika outbreak met with less criticism — the response to Ebola has set the tone for the organization’s own Director-General election that will come July 1. Running for the role are Tedros Adhanom Ghebreyesus of Ethiopia, David Nabarro of the U.K., and Sania Nishtar of Pakistan.
“The new DG (Director-General) will certainly continue to prioritize on-going change and improvements, particularly in health emergencies,” according to a statement WHO provided to CBS News. “You can see this in the platforms of all three candidates.”
“Not the most effective machine”
A lot of the criticisms that WHO faced in its sluggish Ebola response centered on what was perceived as wide-reaching bureaucratic bungling. From the inability to contain a pandemic as it spread easily through porous national borders, to WHO’s conflicts with local governments, the Ebola crisis was the perfect storm of what happens when ineffective institutional practices collide with a deadly infectious disease outbreak.
While facing the brunt of scrutiny, WHO wasn’t the only organization derided for its response to the crisis. For instance, San Francisco-based Metabiota Inc., a company founded to track just this kind of emergency epidemic, was called out for adding to the chaos. A 2016 investigation by the Associated Press revealed that internal warring between company staff members and responders led to some misdiagnosed Ebola cases. The company was chosen by WHO and the government of Sierra Leone to track the virus’s spread.
Dr. Leslie Roberts, a professor of population and family health at the Columbia University Medical Center, was actually on the ground for WHO as its foreign medical coordinator in Sierra Leone during some of the outbreak’s darkest days. Roberts had worked for WHO before — he was an epidemiologist in Rwanda in 1994 during that country’s genocide and civil war.
Roberts told CBS News that he headed to Sierra Leone starting in September 2014 for a three-month period, returning again for about six to eight weeks after his spring 2015 semester teaching obligations at Columbia were finished.
In Sierra Leone alone, there were 8,706 recorded cases of Ebola and 3,956 people died, according to the Centers for Disease Control and Prevention. The highly contagious infection spread from patients to family caregivers and by way of the country’s burial traditions, which involved loved ones rinsing the bodies of the deceased before clothing and often kissing them.
Of course, putting a stop to risky traditional practices can set up a culture clash between a community’s customs and global medical protocols — a difficult balancing act for an organization like WHO, Roberts said. He said this kind of tug-of-war could very easily make the next big pandemic worse.
Roberts said, from his perspective, WHO did an effective job of training responders as well as providing outreach to affected communities. That being said, Roberts acknowledged WHO was “not the most effective machine at stopping this outbreak.”
Pandemics as global security threats
What happens next time a health crisis threatens to spiral out of control?
Moon said an “ideal system” would “see all countries of the world have some basic level of preparedness” when there seems to be a “suspicious pattern of infectious disease.”
But it’s not just about medical practices — some experts say governments need to view pandemics as security threats.
“The Neglected Dimension of Global Security,” a 2016 report from public health officials published by the National Academy of Medicine, looks at how the wave of large-scale infectious disease outbreaks over the past few decades — not just Ebola, but others like HIV/AIDS and SARS — exposed how economically and politically vulnerable nations are in the face of the ravages of future pandemics. The report finds that a range of factors, from growing population numbers to environmental degradation to increasing economic globalization, have shifted the dynamics of how disease outbreaks can affect countries.
“We have not done nearly enough to prevent or prepare for such potential pandemics,” Peter Sands, the commission’s chair, wrote in the preface. “While there are certainly gaps in our scientific defenses, the bigger problem is that leaders at all levels have not been giving these threats anything close to the priority they demand.”
Sands called this the “neglected dimension of global security.”
This report essentially places global pandemics on the same level of seriousness as a military assault on a country.
Since pandemics are generally viewed as “health problems” rather than “security risks,” the study argues that public health departments tend to put outbreak preparedness on the back burner. Rather than building up defenses as one would for a war or a terrorist attack, potential pandemics are relatively ignored.
The commission issued 10 recommendations for building more effective public health resources in countries that are particularly prone to being decimated by an Ebola-level pandemic, such as developing universal benchmarks for preparedness that nations have to meet.
Economic assistance for at-risk countries is also needed —and the report argues that money spent on preparedness would more than pay for itself. For instance, the study contends that if nations invested $4.5 billion a year to safeguard against the next major outbreak, $60 billion a year in losses from future pandemics could be avoided.
The threat of isolationism
When an outbreak emerges, Moon said it’s essential that drugs, vaccines, and diagnostics are “ready to be deployed and ready for people who are affected immediately.” But many financial and geopolitical factors can stand in the way.
“A good example is H1N1,” she said, referring to the global bird flu scare in 2009. “You had some countries actually hoarding vaccine supplies, and some of the vaccines limited in volume did not reach the countries hit hardest by H1N1.”
“We don’t have any system in place still to make sure that doesn’t happen again.”
One potential roadblock she sees is the current rise of nationalism in Western nations that would normally take the lead in developing and distributing vaccines in times of need.
“I’m concerned that this current administration in the U.S. is not concerned about the importance of ensuring that drugs and vaccines could be quickly sent to other places where people are affected,” Moon stressed. “Of course, the reality, ironically, is that this is what is needed to protect Americans around the world. ‘America First,’ if it is going to diminish the need to respond quickly around the world, could hurt other Americans.”
Roberts echoed those thoughts given that much of Europe, including Great Britain, seems to be moving in an “isolationist mindset along with the United States.” He said this could have dire consequences when it comes to public health.
“Eradicating smallpox cost a lot, but it now pays for itself every month. Look, if we could fund for research that would identify multiple drug-resistant strains of pathogens before they show up, or if we could understand, say, Zika, before it comes here — wow. That would make America a lot safer,” he asserted.
“Isolationism is not financially beneficial, and in terms of the risks of outbreaks of disease, it’s not a constructive path for us to be following in this moment of time to keep diseases at bay.”
The cost of a major pandemic could be catastrophic. If an outbreak the scope of the Spanish influenza of 1918 — which resulted in more than 50 million deaths worldwide — were to spring up today, the global economic damage would pile up into the trillions of dollars, on top of the toll in human lives, according to the 2016 commission report.
Moon summed up the shortcomings: “Look, we don’t have good monitoring to actually know how ready or not ready we are. We still need to invest a whole lot more. And there is still the need for more investment to build up WHO’s capacity. WHO remains deeply underfunded in carrying out the pretty big mandate that we, as the world, have put on it.”
“The headline really is: ‘We are not ready.’”