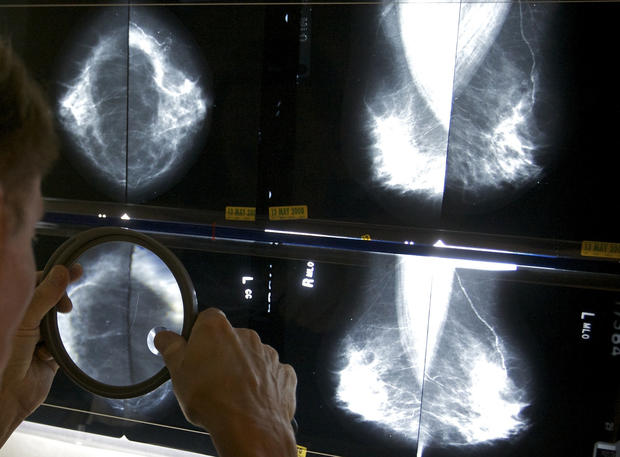
Task force issues breast cancer screening recommendations
When women should begin having mammograms has been a hot topic of conversation in recent years, mainly due to changing -- and sometimes conflicting -- guidelines.
The U.S. Preventive Services Task Force (USPSTF) released its final recommendations for breast cancer screening today in an attempt to clear up some of the confusion.
The group recommends that women at average risk for breast cancer should have a mammogram every other year beginning at age 50 up to the age of 74. Women in their 40s are advised to make an individual decision in partnership with their doctors, since the likelihood of benefitting from screening is lower for women in that age group.
Though this is an update from the group's 2009 recommendations, the guidelines remain largely unchanged and a draft was released earlier this year.
The report, published in the Annals of Internal Medicine, also concluded that there's not enough evidence to determine if newer 3D mammography is a good option for routine screening, or if women with dense breasts need extra testing.
The group's 2009 report drew controversy for questioning the usefulness of mammograms for women in their 40s. But the task force says their words were widely misunderstood.
"Our 2009 recommendation has been incorrectly interpreted as a recommendation against screening for women in their 40s," Dr. Kristen Bibbins-Domingo, vice chair of the USPSTF, said in an accompanying video provided by the group. "Actually the 2009 recommendation and this updated scientific report found evidence that supports a wide range of screening choices."
The American Cancer Society had long recommended annual mammograms starting at age 40, but in new guidelines released in October 2015, the group bumped up the recommended age to begin screening to 45.
Research has shown that starting breast cancer screening at a younger age and screening more frequently is associated with some harms.
"In addition to false-positive tests and unnecessary biopsies, all women undergoing regular screening mammography are at risk for the diagnosis and treatment of noninvasive and invasive breast cancer that would otherwise not cause them harm during their lifetime," Bibbins-Domingo said.
The new guidelines emphasize that when a woman begins regular screening should be an individual one based on her values, preferences, and family history. Women with close relative such as a mother, sister, or daughter with breast cancer, for example, are at a higher risk for the disease and may benefit more than average-risk women from beginning screening in their 40s.
Experts say that the two organizations' guidelines are now fairly similar.
"The USPSTF guidelines... are in many ways aligned with those of the American Cancer Society. We all agree on many points," said Dr. Connie Lehman, director of breast imaging in the department of radiology at Massachusetts General Hospital. "Early detection saves lives and screening mammography has stood the test of time."
Dr. Otis Brawley, chief medical officer for the American Cancer Society, stressed the similarities between the two organization's guidelines and emphasized the importance of screening for women aged 50 to 75.
"We often talk about women in their 40s, but rarely talk about the number of lives that everybody agrees could be saved for women in their 50s, 60s, and 70s who just don't get the screening test," Otis told CBS News. "A third of women 50 to 75 are not getting breast cancer screening. The number of lives that could be saved if we were to work on that one-third of women 50 to 75, get them screened and a good diagnosis."
The American Cancer Society recommends women age 45 to 54 get annual mammograms and those 55 and older switch to screening every two years, or have the choice to continue yearly screening.
The USPSTF determined that more research is needed on whether women should continue screening passed the age of 74.
The task force also said that for the almost 50 percent of women with dense breast tissue, there's not enough evidence to tell if adding additional tests like 3D mammograms or ultrasound exams would improve their outcome. Dense breast tissue makes it more difficult for mammograms to spot cancer, and women with dense breasts have slightly higher risk of developing tumors. Twenty-two states have laws that require women be told if mammograms show they have dense breasts, and some suggest they consider extra testing.
Finally, the task force was unable to make a recommendation on whether or not newer 3D mammograms should be used for regular breast cancer screening, as there is not enough evidence to show if they improve survival and quality of life or worsen over-diagnosis.