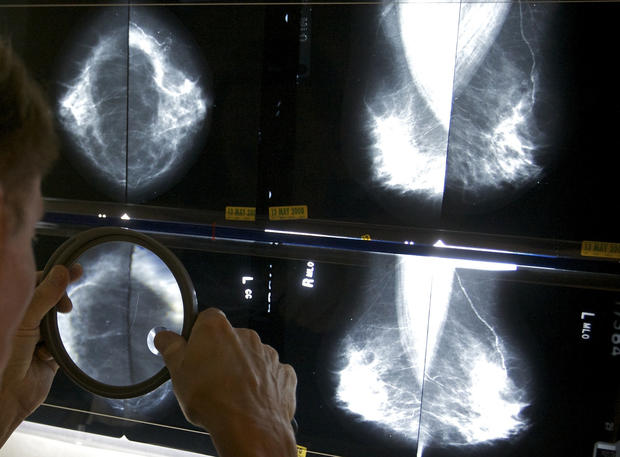
Breast cancer: 6 ways to reduce your risk
By Ilene Manacher
Breast cancer may have touched you or someone you know -- a mother, sister, colleague or friend.
It's the most common form of cancer for women worldwide, and the second most common (after skin cancer) among women in the United States. About one in eight women in the U.S. will develop breast cancer in her lifetime.
October is Breast Cancer Awareness Month, and that finds many women wondering if there's anything they can do to beat the odds.
A lot is out of your control. "Most people who are diagnosed with breast cancer don't have any risk factors aside from being female and getting older," says Susan Brown, Managing Director of Health and Mission Program Education at Susan G. Komen, an organization dedicated to ending breast cancer.
You can't control a family history of breast cancer or having a genetic mutation that increases the risk, although knowing about these can help you make decisions about your health.
But there are some risk factors you can influence.
For one, the trio of obesity, lack of exercise and a high calorie diet are linked to a higher risk of developing not just breast cancer, but any cancer, says Dr. Otis Brawley, Chief Medical Officer for the American Cancer Society.
"Think of it like a three-legged stool," Brawley told CBS News. "The combination already causes nearly a third of all cancers."
Read on for six ways you can reduce your breast cancer risk.
Diet and fitness
"I would encourage women of all ages to try to be physically active and try to maintain a good body weight," advises Brawley. It will lower the risk for breast cancer, and for other serious conditions like diabetes and heart disease.
The relationship between weight and breast cancer is tricky. In younger women, being overweight doesn't seem to be a risk factor; in fact, says Brown of the Komen organization, it might even offer a little bit of protection.
But research shows that gaining weight in adulthood or being overweight after menopause increases the risk for breast cancer after menopause. "Just 20 pounds from the age of 18 is associated with a higher risk of developing breast cancer" after menopause, says Brown.
"The challenge," she cautions, "is that most women who carry extra weight in those pre-menopausal years carry that weight right along with them into post-menopausal years. So just maintaining a healthy weight throughout the lifetime is something that she can control."
And being physically fit counts, too.
"The other thing that lowers the risk of breast cancer is exercise," notes Brawley. The American Cancer Society recommends that healthy adults aim for at least 150 minutes of moderate intensity or 75 minutes of vigorous intensity activity a week.
Limit alcohol
Drinking one glass of alcohol a day is linked to a small increase in the risk of developing breast cancer.
But heavier drinkers, take note: the risk increases with the amount of alcohol consumed. Compared with teetotalers, women who have two to five drinks a day have about one and a half times the risk for breast cancer, according to the American Cancer Society.
On the other hand, you may have heard that alcohol has some benefits. For instance, one study published in the European Heart Journal showed that drinking in moderation can protect a person from heart failure.
Brawley, of the American Cancer Society, notes that the data on alcohol consumption changes frequently. But he says, "if your goal is not to get breast cancer, don't drink."
Having children
If it's an option, there's a benefit to having kids at a younger age.
"We have data to show that women who carry a child to term before the age of 30 have a lower risk of breast cancer than women who do not have a child before the age of 30," says Brawley.
Another benefit: some studies suggest that breastfeeding is also linked to a lower risk of developing breast cancer.
Think twice about hormone therapy
Some women use menopausal hormone therapy, also called hormone replacement therapy, to manage the symptoms of menopause, like hot flashes or dryness. But there's a caution.
"Using menopausal hormones is associated with a higher risk," says Brown.
Specifically, several studies have shown that the use of estrogen plus progestin after menopause, known as combined hormone therapy, increases the risk of developing breast cancer. And the American Cancer Society notes it may also increase the chances of dying from breast cancer.
What to do? Discuss options for managing the symptoms of menopause with a health care provider. If you choose combined hormone therapy, Brown advises "generally the FDA now recommends using that medication at as low a dose as possible for as short a period of time as possible because of its association with breast cancer."
Know your body
The signs of breast cancer aren't the same for everyone. Finding a lump in the breast is a well-known warning sign -- but it's not the whole story.
"A lump in the breast might be a sign of breast cancer, but there are seven other warning signs as well," says Brown.
The important thing is to know how your breasts normally look and feel, and to be alert to changes.
"Knowing what's normal for you - being familiar with your body, and if you notice any changes, see a doctor," says Brown. That's especially important for younger women who aren't generally getting mammograms yet.
The Komen organization urges women to watch out for these eight warning signs of breast cancer:
- A lump, hard knot or thickening in the breast or underarm area
- Swelling, warmth, redness or darkening of the breast
- Change in size or shape of the breast
- Dimpling or puckering of the skin
- Itchy, scaly sore or rash on the nipple
- Pulling in of the nipple or other part of the breast
- Nipple discharge that starts suddenly
- New pain in one spot that does not go away
These signs don't always mean cancer, but if you notice something, get it checked by a doctor.
Discuss screening options
Early cancer detection saves lives, but experts disagree on when and how often to get screened for breast cancer.
For example, the American Cancer Society says women at average risk should have a mammogram every year starting at age 40. They also recommend a clinical breast exam every three years from age 20 and yearly from age 40. There are additional recommendations for women at higher risk, such as those with a family history of breast cancer.
The U.S. Preventive Services Task Force recommends that women between the ages of 40 and 49 who are at average risk should talk to a doctor about the best time to start having a mammogram. For women from 50 to 74, they recommend a mammogram every two years.
What to do? Talk to a doctor about your options.
Brown advises all women, "if they notice a change in their breast or if they learn something about their family history that may impact their personal risk, that they talk to their providers and talk about the types of screening tests that they should be considering."
And, she adds, women should "go and get their screening exams, go and get their mammograms and clinical breast exams as recommended."