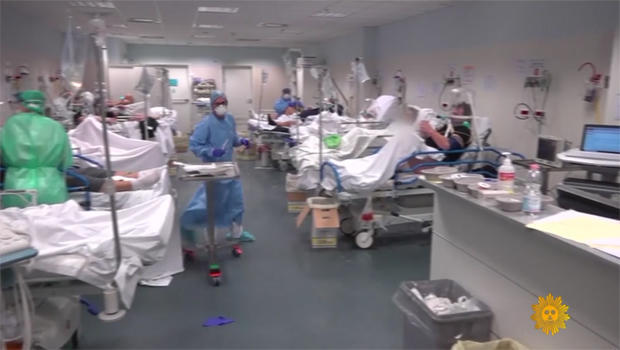
Physicians and bioethicists on a pressing question: Who lives, and who dies?
These are dark times; escalating demands, diminishing resources. To get a sense of where we may be headed, we have only to look at Italy. Theirs is one of the oldest populations in the world, which partially explains a death rate from the coronavirus that is now close to 10%. In the north, Lombardy, the medical system is all but overwhelmed. Too few hospital beds, not enough gowns and masks, a desperate shortage of ventilators.
"Sunday Morning" Senior Contributor Ted Koppel asked Dr. Maria Raven, chief of emergency medicine at the University of California San Francisco Hospital, "You've seen what's happened and what continues to happen in Italy right now?"
"Yeah."
"You've got me on one gurney, and you've got a 25-year-old on another gurney. You've only got one ventilator for the two of us – who gets the ventilator?"
"That's a very tough question," Dr. Raven replied. "I mean, I think the answer that we would use, if we were to follow principles from a specialty like transplants, is that people that have more life years might get the ventilator.
"But there are also many other sort of principles that could underlie the decision-making. You have to take into consideration underlying illnesses that people might have, and you also have to take into consideration if there are other temporizing measures that you could use in one person, so that maybe, after all, you wouldn't have to need a ventilator immediately. So, again …"
"Maria, Maria, Maria … you're tap-dancing!"
"All right, I mean, I can't … this is a tough question," said Dr. Raven. "I mean, I don't necessarily want to speak for UCSF on this, because they haven't put out their guidelines yet."
"When are they planning to put out the guidelines? What are they waiting for?" Koppel asked.
"Well, they're any day. Actually the clinical working group is working on them right now."
These are terrible decisions to leave in the hands of doctors on the front lines – the ones actually treating patients.
"There are certain situations – relatively few, thank goodness – that are catastrophic events that entirely overwhelm our ability to do what's right; Haiti was one of those," said Dr. Thomas Kirsch, an emergency physician sounding the alarm.
- The nightmare of rationing health care by Thomas Kirsch (Washington Post - subscription required)
He's afraid that what he confronted in Haiti in the aftermath of that country's earthquake a decade ago – desperate shortages of medical supplies, equipment and personnel – could soon face us here.
Dr. Kirsch said, "That was the same thing I faced when I was in Haiti. And it's about the most difficult decision that you can make."
"You're still choking up all these years later. Why?" asked Koppel.
"Good question!" Dr. Kirsch laughed. "You know, you think after ten years you'd be beyond that. But it's, again, it's such a difficult decision."
There are guidelines. New York state put out a massive, thoughtful set in 2015. The Italians have drafted a set based on their current experience.
But every hospital follows essentially its own guidelines.
"We're trying to save the greatest number of lives possible," said Dr. Tia Powell, director of bioethics at Montefiore Medical Center in New York. "So in some cases, these guidelines would really shift radically the way we work and put both patients and doctors and families in the terrible position of saying: 'We can't do what you would want.'
"And the basic goal is to divide people into three large categories: One, the lucky group – you have a very mild case, you might feel miserable, but you're not in danger. The group that you're looking for in a hospital is the group that is very sick and that actually may die without critical care resources, but if we can get them those resources they have a good chance of pulling through.
"And then the third group is the most unlucky. That's people with a terrible prognosis, people for whom even with critical care resources the chance of surviving is terrible."
Koppel said, "I'm sure not a term that you will happily use, but we're talking about rationing."
"It's a form of rationing, yeah," said Dr. Powell. "And I agree, everybody tried to avoid that word, but I would actually like people to understand what may be coming."
David Williams, a professor at the Harvard School of Public Health, said, "What we fear will happen, what is most likely to happen, is that persons who are poor, persons who are racial or ethnic minorities, are less likely to get ventilators than those who are wealthy and well-connected.
"And what makes it even more challenging is that the disadvantaged groups we have just talked about, they are the ones who begin this process being more vulnerable, because they have earlier onset of disease, [are] more likely to face chronic, ongoing stressors in multiple domains of their lives. So, we are looking at those most in need being most likely to be disadvantaged."
Dr. Kirsch said, "We have to keep trying and doing things. So, is it likely that people will die from lack of access to ventilators? Probably. Does that mean as an individual patient they're likely to die? No. Because we're not gonna quit trying."
Koppel asked, "So, I understand why you're fighting me on this. You don't want to let anybody believe that the medical community is just gonna give up. And I'm not suggesting that you will. But I am suggesting in the strongest terms that we don't have adequate supplies to meet the likely demand. You don't think that's an unfair statement, do you?"
Dr. Kirsch replied, "Given my knowledge of the situation, that's not an unfair statement. But I'm not a supply guy; I'm a doctor."
Koppel asked Dr. Powell, "Do you think the public is adequately informed about [this]?"
"No, no, no, no," she laughed. "I don't think that the health care community is adequately informed. And I think, you know, experts have been working on this, but now, it is really a realistic possibility. And it's a realistic possibility not in a year but soon. I never thought I would see this day, and we're not quite there. But realistically, many, many health professionals are preparing to do just this."
For more info:
- Dr. Maria Raven, University of California San Francisco Hospital
- Dr. Tia Powell, director of bioethics, Montefiore Medical Center, New York
- Professor David Williams, Harvard School of Public Health
Produced by Dustin Stephens and Deirdre Cohen. Editor: Mike Levine.