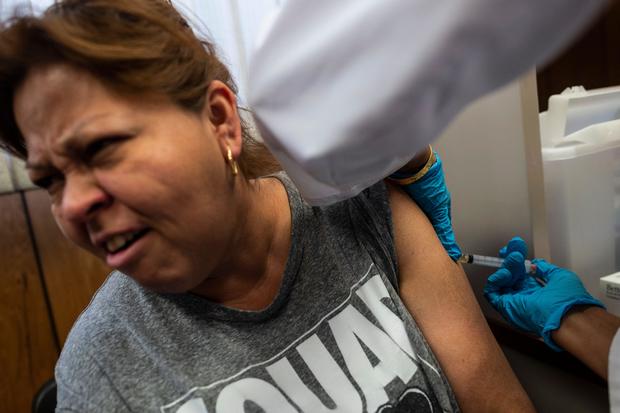
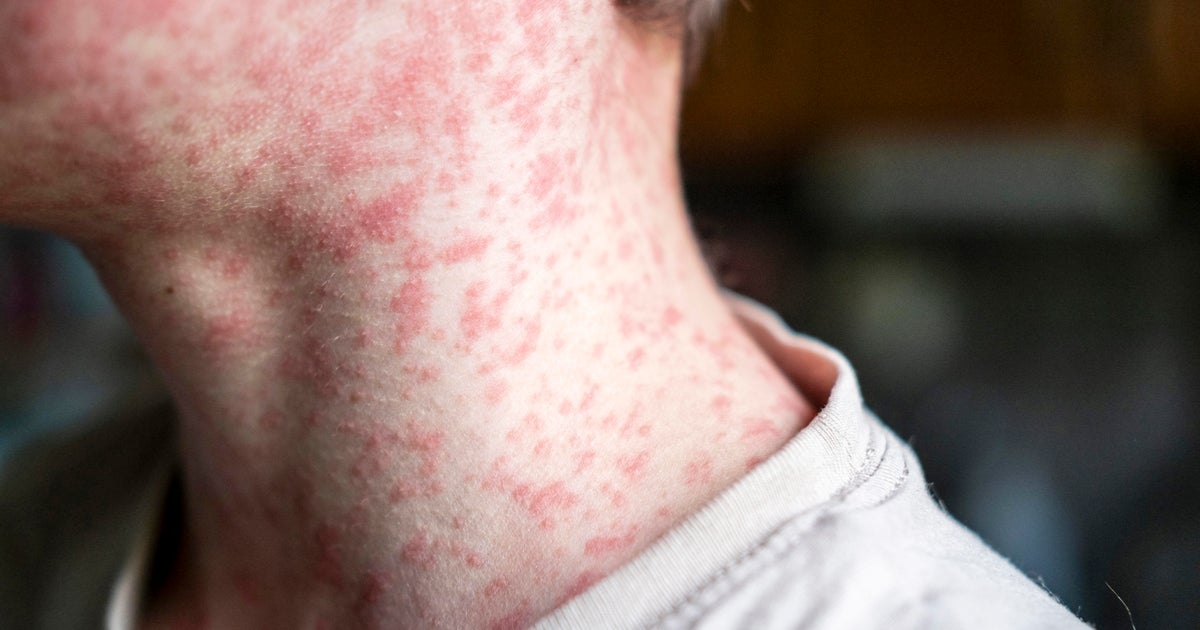
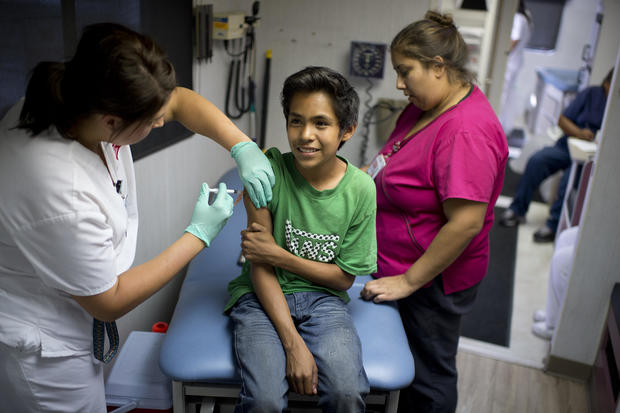35 facts about the measles vaccine
Measles cases in the United States hit a 27-year high in 2019, according to the Centers for Disease Control and Prevention. The CDC said people who were not vaccinated against the highly contagious disease made up the majority of those incidents.
Read on for 35 facts about the oft-misunderstood vaccine — and the potentially deadly virus it fights.
1. Two choices
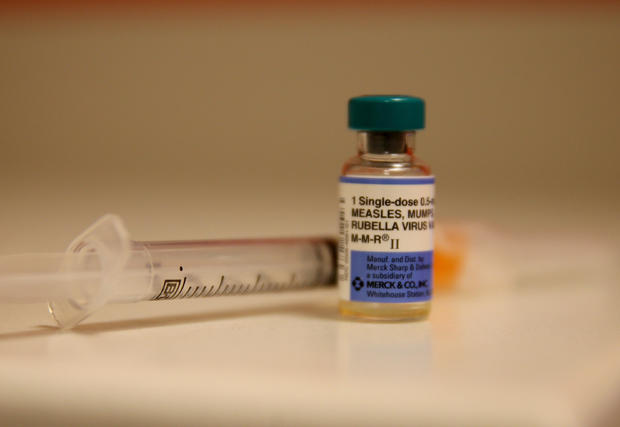
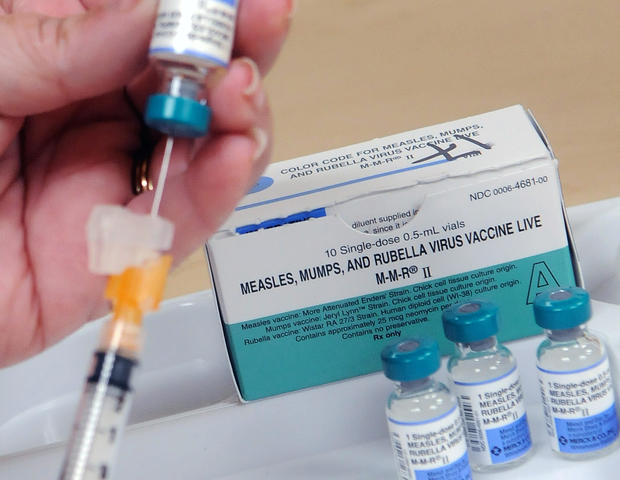
The measles vaccine is administered via one of two combination shots, the measles-mumps-rubella (MMR) vaccine or the measles, mumps, rubella and varicella (MMRV) vaccine.
2. Standard care
The MMR is part of the CDC's recommended vaccination schedule for kids 18 and younger. The shot offers the best protection after two doses, one at ages 12-15 months and the second at 4-6 years.
3. Babies may also need protection
In special cases, the MMR vaccine may be given to a child as young as 6 months. The CDC recommends infants younger than 12 months get their first MMR dose prior to international travel. If a child does receive the MMR vaccine before a first birthday, the CDC says two additional doses — three in total — are needed to confer immunity.
4. Hot spots
Recent measles outbreaks in Los Angeles County, New York and other U.S. metropolitan areas are linked to travelers bringing the disease back from countries dealing with their own outbreaks, the CDC reported. These countries include Israel, the Philippines and Ukraine.
5. Case study
In August 2019, a 43-year-old Israeli flight attendant died of measles-related complications — the third such death in Israel since November 2018. Rotem Amitai was diagnosed with the disease following a flight from New York to Tel Aviv.
6. Measles on the rise
As of Aug. 15, 2019, 1,203 domestic cases of measles, spanning 30 states, were reported to the CDC. By comparison, 372 cases were reported in all of 2018, 120 in 2017 and 86 in 2016.
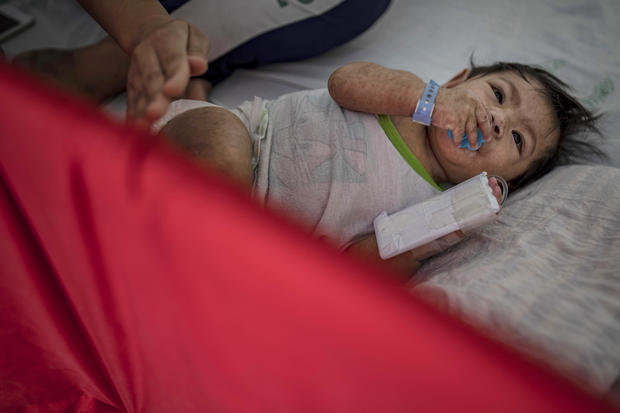
7. Who suffers complications?
According to the CDC, children younger than 5 and adults older than 20 carry the highest risk of complications from measles. Pneumonia, which strikes as many as one in 20 measles-afflicted children, is the most common cause of death among the younger cohort.
8. It may not end with measles
Subacute sclerosing panencephalitis (SSP) is an untreatable, deadly disease caused by the measles virus, but it typically doesn't present itself until perhaps a decade after a person has recovered from measles. SSP is rare, but the CDC says the risk of developing it "may be higher" in people who contracted measles before age 2.
9. Young victims, ultimate toll
Worldwide, measles caused 110,000 deaths in 2017, per the latest data available from the World Health Organization. The majority of the disease's victims were children younger than 5.
10. Big change
Prior to the introduction of the measles vaccine in 1963, an estimated 2.6 million people worldwide died annually from the disease, according to WHO.
11. Agent of change
WHO credits the measles vaccine with preventing 21.1 million deaths worldwide from 2000 to 2017.
12. Big moment
In the United States, measles was declared "eliminated" in 2000. The CDC credited this development to improved measles control — and the measles vaccine.
13. "Elaborate fraud"
In 1998, the British journal The Lancet published a flawed — and ultimately retracted — study that linked the MMR vaccine to autism. The study's author, Andrew Wakefield, would have his medical license revoked and the British Medical Journal would declare his work "an elaborate fraud."
But by then the damage was done: Health officials in the United Kingdom and United States blamed his bogus study for a decline in vaccination rates and a rise in outbreaks.
14. No autism link
A meta-analysis published in 2014 of studies on the possible link between childhood vaccines and autism showed "no relationship" between vaccines and autism. Additional research tracking the health of tens of thousands of people backs up those findings.
15. No link: There's proof
Claims about health risks from vaccines are "based purely on fabrication," Dr. Anthony Fauci, director of the National Institute of Allergy and Infectious Disease, told CBS News in 2019. "That's been proven. There is no association whatsoever between the measles vaccine and autism."
16. Frustrating trend
"These [measles] outbreaks are due to the anti-vaccine movement," Fauci said to CBS News. "When you get below a certain level of vaccination in the community, that's how you get outbreaks."
17. Strength in numbers
The vaccination rate among a target population — children, in the case of the MMR shot — should be between 90% to 95% to prevent outbreaks from spreading, according to the U.S. Department of Health and Human Services. The goal is to "herd immunity" for the entire population, including those too young to get the vaccine.
18. States falling short
According to a CDC report on MMR vaccination rates among children ages 19 to 35 months, several U.S. states in 2017 fell short of the 90% to 95% immunization goal. Alaska, Colorado, Indiana, Missouri, New Jersey, Ohio, South Carolina, Utah, Washington and Wyoming all failed to top 89.3%.
19. Getting the job done
U.S. states with the highest MMR vaccination rates in 2017 per the CDC study included Massachusetts, North Dakota and Virginia. All three states boasted immunization rates north of 95%.
20. Loopholes
According to the National Conference of State Legislatures, all 50 states legally require vaccines for school-aged children. But, as of June 2019, only California, Mississippi and West Virginia will not grant exemptions to those rules for religious and personal-belief grounds.
21. On the feds' radar
In February 2019, U.S. Food and Drug Administration Commissioner Dr. Scott Gottlieb warned that the federal government may step in if states don't close their vaccination loopholes.
22. No spread
People who have been vaccinated against measles cannot transmit the disease to someone else.
23. A small price
According to the World Health Organization, it costs about $1 to immunize a child against the measles.
24. Mild side effects
According to the CDC, the MMR vaccine is not only "very safe," but "much safer" than getting the measles. Common side effects from the shot run on the mild side: a sore arm at the vaccination site, fever, a mild rash, and temporary joint pain and stiffness.
25. Less-common side effects
The MMR vaccine presents a "very small risk," of causing fever-induced febrile seizures, according to the CDC. Febrile seizures can look scary, but are typically harmless. Serious allergic reactions to the MMR vaccine are also considered "extremely" rare.
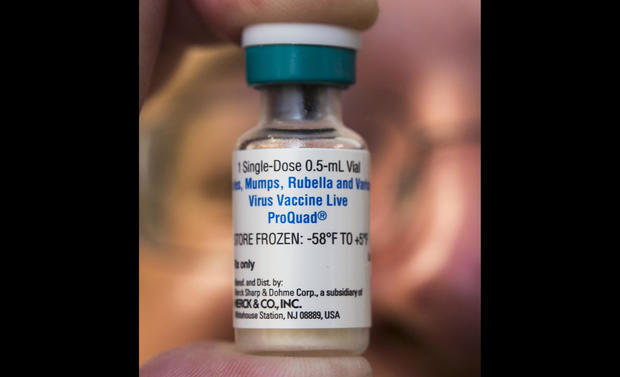
26. The other shot
The MMRV, which additionally protects against varicella, commonly known as chickenpox, is a two-dose vaccine. As with the MMR, it is recommended that the first dose be administered to children beginning at 12 months.
27. Balancing act
Because MMRV bundles the chickenpox vaccine, it means children can get away with one less shot over the course of their vaccinations — and that can be a big deal for the needle-adverse.
The MMRV, however, does come with an increased risk of fevers: Roughly 22 out of every 100 children will run a fever of 102 degrees or higher, post-vaccination, per the CDC. The MMR results in fevers in about 15 out of every 100 children.
28. Rare seizures
Febrile seizures are more common with the MMRV than with the MMR, but they're rare outcomes with both shots: About eight of every 10,000 children will suffer a febrile seizure in the five to 12 days after the MMRV shot is administered. With the MMR, the stat line is roughly four out of every 10,000 children.
29. New kid on the block
The MMR is the older measles vaccine shot: It was introduced in 1971, while the MMRV was approved by the U.S. Food and Drug Administration in 2005. Like the MMR, the MMRV is considered "very safe" by the CDC.
30. Not just kid stuff
If you received the measles shot between 1963 and 1968, in the vaccine's earliest days when it wasn't as reliably effective, you may need a booster shot.
31. Baby-boomer rule
If you were born before 1957, when measles was prevalent, then according to the CDC you do not need the measles vaccine as you were probably naturally infected with the virus. But only laboratory blood tests will be able to confirm your immunity status.
32. Check up
The CDC recommends MMR shots for adults, regardless of age, who work in health care and who don't have lab work proving immunity. Other high-risk adults who should check with their doctor about needing a booster: college students and international travelers.
33. Only game in town
Adults who need a measles shot need the MMR; the MMRV is not licensed for use in those older than 12. Children younger than 12 months can't get the MMRV, either.
34. Fetal issues not included
Despite some beliefs to the contrary, vaccines, such as the measles shots, do not contain fetal tissue. The MMR and MMRV also do not and have never contained thimerosal, a mercury-based preservative that has been judged safe in low doses, but that was nonetheless removed as an ingredient from all childhood vaccines in 2001.
35. Words of warning
The WHO considers "vaccine hesitancy" — the reluctance or refusal to immunize — as one of the top 10 threats to global health in 2019.