How to treat - and avoid - summer skin problems
Few things are more maddening than an itch. And summer is prime time for all kinds of creepy-crawly sensations, often accompanied by mysterious lumps, bumps, cracking, crusting, swelling, and oozing (delightful!).
"Most itching has an obvious cause, such as bug bites or dry skin," says Dr. Ronald Brancaccio, director of the Skin Institute of New York and clinical professor of dermatology at New York University School of Medicine. "But sometimes an itch or the rash that goes with it can be hard to figure out, even if it has a straightforward cause like an allergic reaction."
Keep clicking as our friends from Health.com uncover common summer skin problems...
More from Health.com: 8 steps to healthy skin at every age
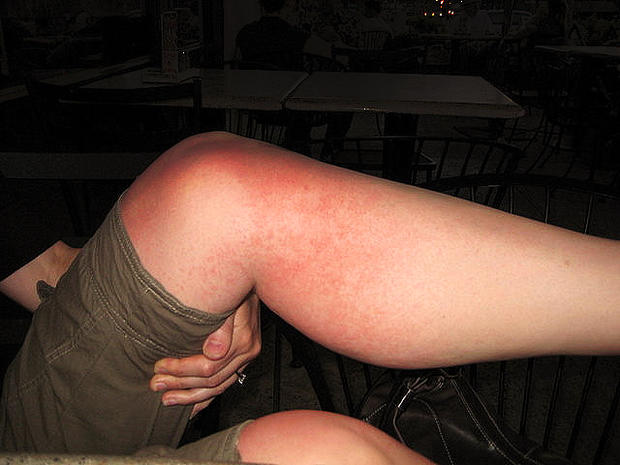
Heat rash
Hot, humid weather brings on this rash, in which clogged sweat ducts trap perspiration under the skin. It shows up as tiny, itchy bumps or blisters, most often in skin folds or places where clothes cause friction.
Treat it: Heat rash usually goes away on its own after a few days. Wear lightweight, breathable fabrics to allow sweat to evaporate, and avoid heavy creams or ointments that might block sweat ducts.
See your MD...if the rash lasts for more than three to four days, gets worse, or if you have signs of infection, such as fever or increased pain, swelling, or redness.
More from Health.com: 8 steps to healthy skin at every age
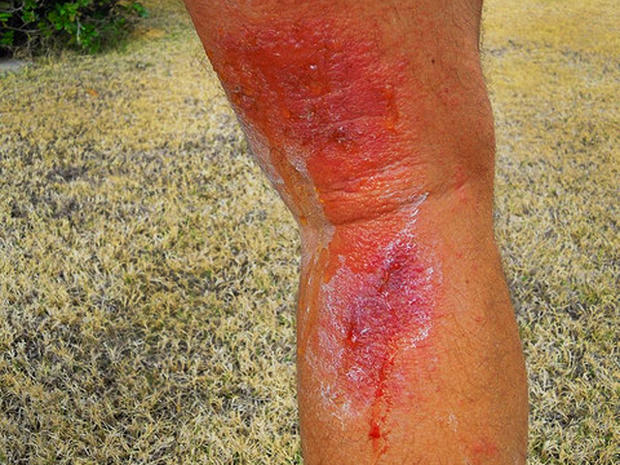
Poison ivy
Technically, it's not poisonous. But an estimated 85 percent of people are allergic to the urushiol oil in poison ivy, poison oak, and poison sumac. Brushing up against one of these creepers can result in red raised patches, often with blisters, swelling, warmth, and, of course, itching. The reaction usually appears 12 to 72 hours after exposure.
More from Health.com: 8 steps to healthy skin at every age
Poison ivy: Treat it
Your first line of defense: Wash right away with soap and water to remove the irritating oils. (Also wash clothes, shoes, even pets - anything that could have come in contact with the plants or their oils.) Topical OTC corticosteroids (like hydrocortisone) can reduce swelling and help skin heal faster. Relieve itchiness with cold compresses, calamine lotion, and/or an oral antihistamine.
See your MD...if you have a severe reaction or if the rash covers more than 10 to 20 percent of your body. Also see your doc if the rash doesn't clear up after two to three weeks, gets worse, or seems to keep recurring - you could be allergic to something else in your environment.
More from Health.com: 8 steps to healthy skin at every age
Yeast infection
You already know that warm, moist conditions can contribute to a vaginal yeast infection, caused by an overgrowth of a fungus called Candida albicans. It can also develop when the acidic balance in the vagina shifts, such as after you've taken antibiotics or steroids, during pregnancy and menstruation, and when taking birth control pills.
More from Health.com: 8 steps to healthy skin at every age
Yeast infection: Treat it
If this isn't your first yeast infection, and you recognize the symptoms (redness, swelling, itching and irritation, and/or a white, clumpy vaginal discharge), go ahead and use an OTC treatment.
See your MD...if you've never had a yeast infection before (or if you're at all unsure). Your doctor can determine if it's something else, such as bacterial vaginosis (the most common vaginal infection among women of childbearing age) or a sexually transmitted disease.
Also check in with your gyno if the condition doesn't clear within a week or returns within a month.
More from Health.com: 8 steps to healthy skin at every age
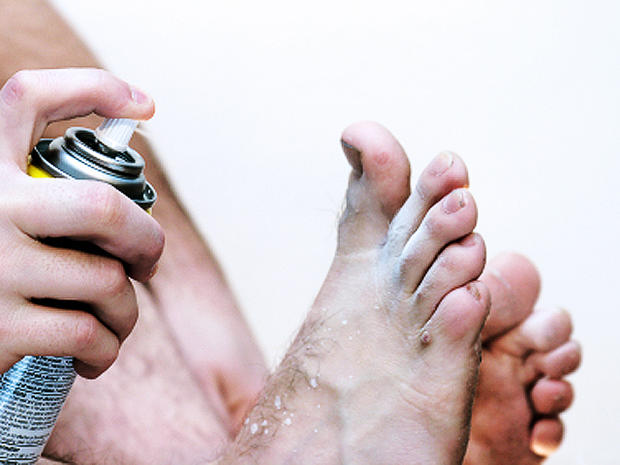
Athlete's foot
The name conjures up grimy locker rooms, but you can get athlete's foot even if you'd never dream of strolling around barefoot at the gym. This fungal infection can take hold if your feet get sweaty in closed-toe shoes, if you have a minor skin or nail injury, or even if you get a pedicure with poorly sterilized tools. Its calling card: cracked, flaking, peeling skin between the toes, along with oozing and crusting blisters.
Treat it: Apply OTC antifungal creams (Lamisil, Lotrimin) as directed until the condition clears.
See your MD...if it turns into a nail infection, or if symptoms persist for a few weeks. Your MD can prescribe an antifungal cream or pill.
More from Health.com: 8 steps to healthy skin at every age
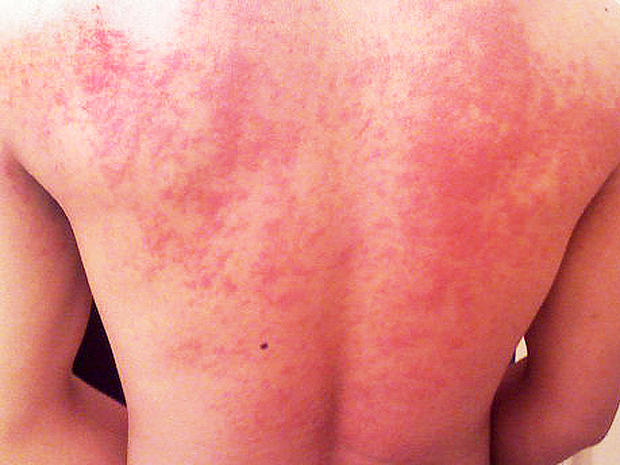
Hives
Hives are a common reaction to many different allergens, including animal dander, insect bites, medications, pollen, or foods, as well as infections (such as mononucleosis). Occasionally, they pop up when you're stressed, exposed to extreme cold or sun, or sweating profusely.
The raised red welts with clearly defined edges can appear anywhere on the body; they may get bigger and spread and merge with other welts, and can disappear and reappear.
More from Health.com: 8 steps to healthy skin at every age
Hives: Treat it
Mild hives may disappear on their own within hours. Calm itching with an antihistamine (such as Benadryl or Zyrtec). Avoid hot showers and tight-fitting clothing.
See your MD...if mild hives don't respond to antihistamines - your doc may want to rule out other illnesses or refer you to an allergist. Call 911 if hives are severe or you have signs of anaphylaxis (a life-threatening allergic reaction), such as fainting, tongue or face swelling, shortness of breath, tightening of the throat or wheezing.
More from Health.com: 8 steps to healthy skin at every age