What the AHCA's preexisting condition rules could cost you
Health insurance coverage for people with preexisting conditions is at the center of the debate over the Republicans' American Health Care Act. Passed Tuesday by the House of Representatives, the legislation is now in the hands of the Senate, where it's expected to undergo major changes.
One of the biggest areas of concern is the AHCA's provision that allows states to obtain waivers for the Affordable Care Act's requirement that insurers must accept people with preexisting conditions and charge them the same premiums as healthy people of the same age. States that apply for and receive such waivers may use federal funds to set up state government-operated insurance programs called high-risk pools to cover patients with health issues who have let their insurance policies lapse.
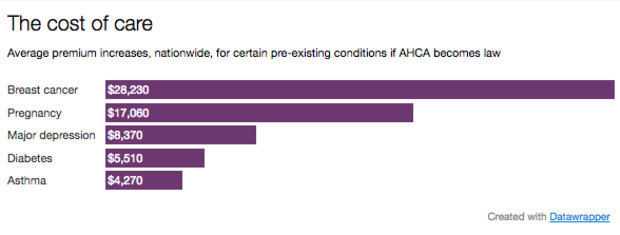
For sick patients in such states, premium costs could skyrocket, according to a report from the Center for American Progress. On average, a 40-year-old with asthma would pay $4,270 more in premiums, while someone the same age with breast cancer would pay $28,230 extra.
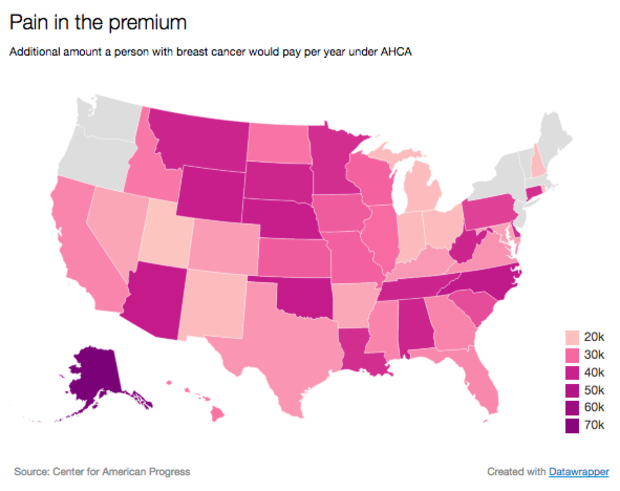
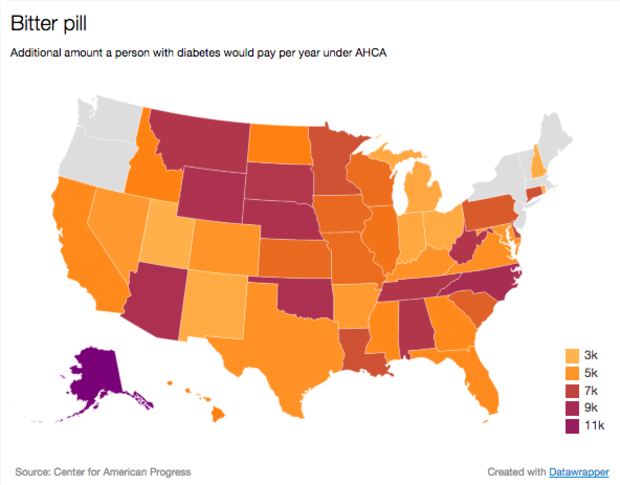
Costs vary by state. For example, according to the study, the breast cancer patient in Alaska would pay $76,000 more in premiums, far higher than the national average, while the asthma sufferer in Utah would pay $2,750 more, less than the national average.
Seven states have preexisting condition protections that would help avoid these increases. Maine, Massachusetts, New Jersey, New York, Oregon, Vermont and Washington all prohibited so-called health status underwriting before the Affordable Care Act was passed.
Proponents of the AHCA defend the waiver, saying that health care decisions are better made by local officials than mandated by the federal government. The waiver, they say, gives states the flexibility to manage health care costs how they see fit.
In addition, Health and Human Services Secretary Tom Price explained that protections for patients with preexisting conditions would remain in place because states applying for a waiver would have to prove they will provide "better coverage for older and sicker patients."
To that end, an amendment to the AHCA provides for more government funds to be made available for "high-risk pools." Under the House legislation, an additional $8 billion over five years will be allocated for these state-run insurance pools. That brings the total to about $138 billion over a decade set aside for high-risk pools and other efforts to stabilize insurance markets.
Nonetheless, critics of the legislation -- which in a rare alliance include Democrats, doctors, hospital executives and even some insurance company executives -- worry that not enough money is allocated to properly fund high-risk pools. An analysis from health advocacy group Families USA finds that the increase would still leave behind as many as 15 million people with preexisting conditions.
At the same time, The Commonwealth Fund has estimated that risk pools would need about $178 billion to cover everyone with preexisting conditions, well more than the amount earmarked by the new legislation.
In an interview with California Healthline, CEO Paul Markovich of Blue Shield of California worried that the AHCA "could return us to a time when people who were born with a birth defect or who became sick could not purchase or afford insurance."
Critics also point to other flaws that existed in the previous risk pool system, including long wait lists and abrupt discontinuation of coverage due to individual states' inability to predict health costs for patients who require expensive treatments. In the 30-plus states that had high-risk pools in 2011 (before Obamacare took full effect), net losses piled up to more than $1.2 billion, or an average of $5,500 per person enrolled.
Preexisting conditions aside, critics of the AHCA also worry about premium increases for all but the youngest people seeking insurance. Because of the legislation's flat-fee, age-based structure of tax credits designed to offset health insurance premium costs, older Americans are expected to receive far less in subsidies than they did under the ACA, meaning their share of premium payments will rise.
What's more, some experts believe people who purchase health insurance through their employer may also stand to lose because of the waiver provision.
That's because states receiving a waiver may also be exempt from other federal health insurance regulations such as lifetime limits on coverage and caps on out-of-pocket costs. Large employers aren't obligated to follow the rules in their own states where they're headquartered but may choose another state. If an employer opts for a waiver state, it would be free to impose some or all of these restrictions on its plan to defray costs.
The Associated Press contributed to this report