Nowhere to Go: Mentally ill youth in crisis
The following script is from "Nowhere to Go" which aired on Jan. 26, 2014. Scott Pelley is the correspondent. Michael Rey and Oriana Zill de Granados.
Last November
19th, Virginia State Senator Creigh Deeds was slashed and stabbed repeatedly by
his own son. Gus Deeds was 24 years old and had been struggling with mental
illness. He and his father had been in an emergency room just hours before the
attack but didn’t get the help that they needed. The story of what went wrong
with his medical care exposes a problem in the way that America handles mental
health. It’s a failure that came to the fore with the murders at Sandy Hook
Elementary School.
Creigh Deeds: I really don't want Gus to be defined by his illness. I don't want Gus to be defined by what happened on the 19th. Gus was a great kid. He was a perfect son. It’s clear the system failed. It's clear that it failed Gus. It killed Gus.
We met Creigh Deeds four weeks after the attack. He was still distraught. But he told us his story was a warning that could not wait.
Scott Pelley: What would have saved Gus?
Creigh
Deeds: If he could have been hospitalized that night, they could have gotten
him medicated, and I could have worked to get Gus in some sort of long term
care.
"I really don't want Gus to be defined by his illness. I don't want Gus
to be defined by what happened on the 19th. Gus was a great kid. He was a
perfect son. It’s clear the system failed. It's clear that it failed Gus. It
killed Gus."
This is Gus Deeds when he was 20 years old, a talented musician on the Dean’s List at the College of William and Mary.
Creigh Deeds: Gus, when he turned 20, I was running for governor. He wanted to come and so he took the fall of 2009 to be with me and those are some of the best memories of my life is having him with me there.
Creigh Deeds: Gus had posted weird things on his Facebook page about-- you know, how the professors were ganging up against him. And he was gonna start boycotting class. It was pretty clear to me that he wasn't taking medicine. I told Gus that he and I needed to talk to somebody together.
That’s when Deeds discovered that "talking to somebody," getting treatment, is harder in mental health than any other kind of medicine. In the decades after the 1960s most large mental institutions were closed. It was thought that patients would get better treatment back in their communities. But adequate local facilities were never built. The number of beds available to psychiatric patients in America dropped from more than half a million to fewer than 100,000. That leaves many kids in crisis today with one option: the emergency room.
Brian Geyser: You know, every day, we have 10 to 20 kids with psychiatric problems come into our emergency department, kids who wanna kill themselves, who’ve tried to kill themselves, who've tried to kill somebody else.
Brian Geyser is a nurse practitioner we met in the emergency department of Yale New Haven Hospital in Connecticut— it’s one of the best in the nation in psychiatry.
Brian Geyser: We have 52 psychiatric beds here at Yale. And right now, all 52 are full. And so the seven kids that are here in the emergency room are waiting for an open bed.
Scott Pelley: How long will they wait?
Brian Geyser: Five of them have been here three days already.
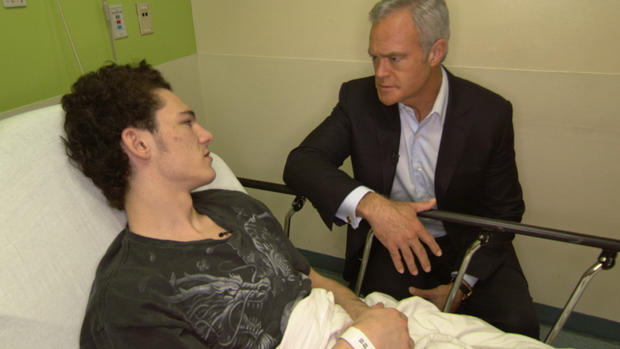
Most every day the beds are full of patients in crisis. Seventeen-year-old Tyler Wrightington was waiting in the ER. He had just slashed his face with a knife.
Tyler Wrightington: Yes. A new voice came about a year ago. And he, well, I call it a he, 'cause it was more of a deeper voice. But he ended up telling me to hurt myself and making me find ways to hurt myself.
Scott Pelley: Do the voices ever tell you to hurt someone else?
Tyler Wrightington: Only once, and that was at school. And they and that was when I got admitted into the hospital. 'Cause I was actually considering hurting the people around me. And I was, I was like, "This ain't me. This is not what I wanna do."
Tyler’s dad, Ernie Wrightington, had called a psychiatrist that week but couldn’t get an appointment for three months. There’s a national shortage of psychiatrists.
Scott Pelley: Why is there not another option for you?
Ernie Wrightington: This has always been our only option.
Scott Pelley: The emergency room.
Ernie Wrightington: The emergency room, yeah. Because the, we know that when we come here, they take the time to take care of him. They sit and watch him, make sure he's OK.
But OK usually means— OK for the moment. Typically, insurance companies pay for this care only as long as the patients are – quote -- at “imminent risk” of harming themselves or others.
Brian Geyser: Some insurance companies will give us a couple of days, a few days before they ask us to call them back to get reauthorization for the admission. Some of them are every single day that we have to call. And so usually, you know, we're talking about, you know, three to four days, and the insurance companies are saying, "All right, you know, it's time. Let's get this kid out."
Scott Pelley: Because they're not going to kill themselves or someone else right now?
Brian Geyser: Right now, yeah.
Many patients need care for months or years. But there are few facilities of that kind, they’re expensive, and often insurance won’t cover them. So kids in crisis spin in the emergency room’s revolving door.
Brian Geyser: We need to be able to set up a system where we follow these kids into the community, we follow the families, we make sure that they have a safety net, and somebody's watching them and monitoring them because, you know, it could be next month, it could be six months from now, and the child will do something again, but if they are not hooked into a system that is watching them, taking care of them, then we could have problems on our hands.
Scott Pelley: How many of you have had to take your child to the emergency room? Everybody.
Scott Pelley How many times?
Mary Jo Andrews: I can't count.
Meg Clancy: I couldn't count.
Seven Connecticut mothers, including Mary Jo Andrews, Meg Clancy, and Dee Orsi told us about their ER crises and battles over insurance.
Dee Orsi: My daughter, after spending, she was eight old at the time, spending 12 days in the hospital they told me she was ready to come home. By Friday morning we were in the psychiatrist’s office for her follow up appointment. She was seeing blood dripping from the walls. There were statues telling her to kill me and she was ready for discharge three days earlier.
Meg Clancy: We had one with an insurance company. They wanted to discharge my daughter. She needed to stay where she was safe and the insurance company would not pay and so I was told by our social worker in the hospital that if I gave my daughter up to Department of Children and Families, that then she would have insurance coverage through the state and she would be allowed to stay.
Scott Pelley: Wait a minute. Give-- give--
Meg Clancy: Give her up.
Scott Pelley: Give her up to the state?
Meg Clancy: Correct. Give her up to the state.
Scott Pelley: And you said what?
Meg
Clancy: Absolutely not.
"They wanted to discharge my daughter. She needed to
stay where she was safe and the insurance company would not pay and so I was
told by our social worker in the hospital that if I gave my daughter up to
Department of Children and Families, that then she would have insurance
coverage through the state and she would be allowed to stay."
They formed this support group because so few people understand their troubles. For example, they share the names of contractors to repair walls or remove doors. Their children punch holes in the dry wall and can’t be allowed to lock themselves in a room.
Scott Pelley: What is the difference between being the mother of a child who has mental illness and the mother of a child who might have heart disease or cancer?
Meg Clancy: Sympathy.
Being in Connecticut, they watched the tragedy at Sandy Hook Elementary with more insight than most. Referring to the killer’s mother one of them told us, if Nancy Lanza had a health care plan for her son, “she couldn’t have made it work.”
Mary Jo Andrews: There’s really no place after the hospital so the kids end up coming back home right where the situation started. And you know, the psychiatrists and the hospital will say, "You’re right, the system is broken" and I remember at one discharge I refused to sign the discharge paper because I wasn’t going to agree that it was appropriate.
Scott Pelley: They discharged your child anyway?
Mary Jo Andrews: Oh yeah, yes.
That is essentially what happened to Creigh Deeds in Virginia last November. But his effort was further complicated by the fact that his son Gus was an adult, over 18—and Gus didn’t want treatment. Deeds had to get a court order and sheriff’s deputies to take Gus to the ER. A state law, designed to protect patients’ rights, meant that the court order would expire in only six hours. That’s all they had to find a hospital that would admit him.
Creigh Deeds: Whole afternoon, Gus didn't sit down. He paced the floor. He'd look at me. He'd smile. And I just had this sinking feeling that he wasn't gonna be hospitalized.
Scott Pelley: And if you didn't find a hospital bed in six hours, Gus was comin' home.
Creigh Deeds: He was coming home. And I was concerned that if he came home, there would, there was gonna be a crisis.
A representative of the county agency that manages mental health care told Deeds that he couldn’t find a hospital with a psychiatric bed appropriate for Gus’ case.
Scott Pelley: You're concerned that your son is suicidal-- the clock has run out on the emergency room and he comes in and says, "Sorry, you've gotta leave?"
Creigh Deeds: Well, the-- he said that Gus wasn't suicidal. I guess he'd made--
Scott Pelley: Based on his evaluation.
Creigh Deeds: His evaluation that Gus wasn't suicidal.
Scott Pelley: What did you say to him, in leaving--the emergency room?
Creigh Deeds: I said, "The system failed my son tonight."
There was no place to go but home.
Scott Pelley: He attacked you.
Creigh Deeds: Twi-- he-- he-- he got me twice, you know, stabbed me twice.
Scott Pelley: With a knife?
Creigh Deeds: The state police told me they found a knife. I turned around and said, "Bud, what's going on?" I said-- and he just kept coming at me. I said, "Gus, I love you so much." I said, "Don't make this any worse than it is." He just kept coming at me. And he just kept-- I mean-- you know-- I-- and I-- I was-- I was-- I was bleeding a good bit but, you know, he turned around and he started walking toward the house.
Deeds staggered away. A neighbor found him. A helicopter ambulance was called.
Creigh Deeds: When I was in the rescue squad or in the helicopter somewhere I'd heard about some, you know, some call came over the scanner that there'd been somebody with a gunshot wound to the head.
Scott Pelley: The gunshot victim was Gus.
Creigh Deeds: Oh, yeah.
Gus killed himself. He had found or bought ammunition for that last rifle, the unloaded rifle, that Deeds had kept in the house.
Scott Pelley: You were describing the last night in which he was writing feverishly in this notebook before you said good night. Did you go back and look at that?
Creigh Deeds: I did.
Scott Pelley: What was he writing?
Creigh Deeds: He had determined that I had to die, that I was an evil man-- that he was gonna execute me and then he was gonna go straight to heaven.
Creigh Deeds has now returned to the Virginia Senate. He’s introduced bills to, among other things, extend emergency custody in an ER from six to 24 hours and to create a computer database to list all the open psychiatric beds statewide.
Creigh Deeds: There’s just a lack of equity in the way we as a society, and certainly as a government and insurance industry, medical industry, with the way we look at mental health issues.
Scott Pelley: Don't want to fund it. Don't want to talk about it. Don't want to see it.
Creigh Deeds: Absolutely. That-- that's exactly right. But the reality is, it's everywhere.
Scott Pelley: You've told us in this interview again and again that you don't want Gus to be defined by what happened in those few seconds on that day.
Creigh Deeds: I want people to remember the brilliant, friendly, loving kid that was Gus Deeds. We'll use Gus, I hope, to address mental health and to make sure that other people don't have to suffer through this.
The state of Virginia is investigating why there was no hospital bed for Gus Deeds that night. Nationwide, since 2008, states have cut $4.5 billion from mental health care funding.
Editor's Note: Families in need of help with a mentally ill child can find resources at the National Alliance on Mental Illness: www.nami.org or 1 (800) 950-NAMI (6264).