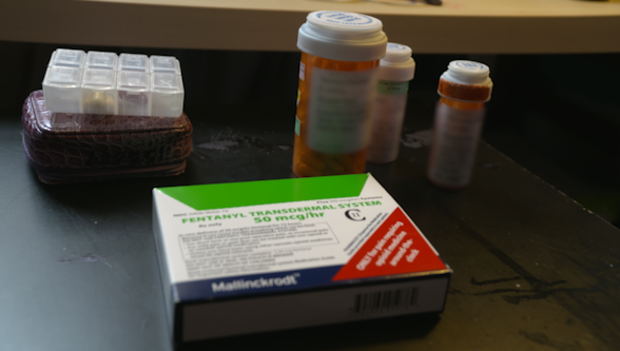
As U.S. grapples with opioid epidemic, new ways to fight pain and addiction
NEW YORK - Retired New York City bus driver Ronald Ruiz, 70, clutched a wooden cane and occasionally grimaced with pain as he shuffled with difficulty around the cluttered, colorful house he had lived in his whole life.
"It's like a pulling, sort of like a tearing, of my back. Any movement makes me feel like somebody's pulling two different ways to look at my spine, like they're pulling my skin apart," said Ruiz, lifting his shirt to expose three deep scars along his back, the vestiges of two spine surgeries, in 2010 and 2014.
"I roller-skated, played hockey, rode a bike from one borough to another. I don't think there was anything I couldn't do - and didn't do. I used to go to Coney Island--" Ruiz cut off mid-sentence, as his face crumpled and voice broke.
"I get emotional because - I don't do anything," he said, fighting back tears. "It's tough. Real tough."
According to the National Institute on Drug Abuse, 116 million Americans, like Ruiz, suffer from chronic pain. Ruiz has been fighting pain with prescription opioid painkillers for nine years, namely Oxycodone.
He said his current dose was "down" to six 30-milligram tablets daily.
"And I'm almost ashamed to say it, because every day in the paper I read about more people who are on it for different reasons," said Ruiz. "I am addicted because - the addiction of it, I need to have a life. And the pain medications that they're prescribing today are addictive."
Ruiz described feeling a sense of guilt and stigma associated with his addiction to prescribed opioid painkillers, since he felt it lumped him in with the broader opioid epidemic plaguing America, including the rise of heroin as a cheaper alternative to opioids like Oxycodone.
"I'm horrified, absolutely horrified - because I feel like I'm almost a part of it," he said. "And I don't want to be a part of - that."
Painkillers and the cycle of addiction
Prescription drug abuse, namely the rise in opioid-related overdose deaths, is considered the fastest growing drug problem in the United States, according to the Journal of Medical Regulation. Opioids were involved in about two-thirds of all the 47,055 drug-overdose deaths in 2014, and 18,893 of those were associated with prescription opioids, according to the the Centers for Disease Control and Prevention (CDC). More recently, there has also been a surge in drug overdose deaths involving heroin and synthetic opioids like fentanyl and tramadol. A January 2016 CDC report linked the rise in illicit opioid overdose deaths to the 15-year trajectory of overall rising overdose deaths involving prescription opioid pain relievers.
"The more that opioids are used to treat pain, the more is there an increase in pain," Connie Greene, vice president of the New Jersey-based Barnabas Health Center for Prevention, told CBS News. "The pills and medication is very expensive, and heroin is very cheap, so we're looking at a population that's addicted because of pain medication and a population that's addicted because of street drugs."
Heroin overdoses have more than tripled in the past four years, while overdoses linked to prescription painkillers doubled in that same period.
"More than 40 Americans die each day from prescription opioid overdoses, we must act now," said CDC Director Tom Friedman in a statement. "Over-prescribing opioids - largely for chronic pain - is a key driver of America's drug-overdose epidemic."
Seated behind her large desk in the Barnabas Health office headquarters in Lakewood, New Jersey, Greene said part of the problem of fighting the opioid epidemic lies in the subjective nature of addiction and pain treatment.
"We're talking about the most abused drugs in this country are used for both anxiety and pain - and [for] both of those, medications is determined the subjectivity of a patient, and what they consider the level of pain to be," she said.
The federal government's Substance Abuse and Mental Health Services Administration found that, in the past year, more than 11 million people aged 12 and above misused opioids, both pain relievers and heroin.
"So that's part of the problem, that people were self-prescribing," said Greene. "Because if my level of pain is 10, my doctor has to do something to address that level for me. And it was the opioids that worked best."
Greene said that opioids became a "quick fix," but that the scope of the opioid epidemic, and the pathway from painkillers to opioid addiciton and heroin necessitated a different approach.
"We as a hospital system, we need to look at other methods of dealing with pain," Greene said.
Community approaches to fighting the cycle of pain and addiction
In addition to President Obama's National Drug Control Strategy, implemented initially in 2010, the White House recently pledged to spend an additional $2 billion over the next two years to fight heroin and opioid addiction, mainly through medication-assisted treatment, like methadone clinics, on a state-by-state basis, involving an expansion of state-level prescription-drug overdose prevention strategies.
This kind of state-led, behavioral-health driven approach is what Greene's Barnabas Health program is spearheading in New Jersey, where heroin and opioid admissions to recovery programs accounted for around half of all substance abuse admissions in 2015, the highest in at least a decade, according to the state Division of Mental Health and Addiction Services.
In 2014, more than 600 people died of heroin-related overdoses in New Jersey, doubling the amount of deaths from the drug since 2011, according to the state Medical Examiner's Office.
Last January, Barnabas Health implemented the Opioid Overdose Recovery Program in Monmouth and Ocean counties, which were among the counties with the highest number of opioid overdose deaths in the state in 2014. The program works in partnership with law enforcement and health care providers including five hospitals, through grant funding provided by the New Jersey Department of Human Services, Division of Mental Health and Addiction Services (DMHAS). It relies on 15 recovery specialists who work with law enforcement and health care systems across five hospitals to reach individuals who were revived from an opioid overdose.
Angela Cicchino, a twenty-something former addict and Barnabas recovery specialist, spoke to CBS News on a recent afternoon, in the Monmouth Medical Center hospital in Lakewood, New Jersey, across the street from Greene's office.
"We come into a room like this, and a lot of the time the family members will be here, maybe outside of the room - sometimes we've had patients who don't have anyone here, they're kind of at the end of the road," Cicchino said. "As a recovery specialist we're trained to get the temperature of all of that: like what's going on, what is their life, what brought them to this place?"
When an overdose occurs, whether heroin or prescription pain medication, first respondents increasingly use a drug called Narcan, a nasal spray that was previously available through a needle or auto-injector, and reverses an opioid overdose. In May 2013, New Jersey Governor Chris Christie signed into law the Overdose Prevention Act, permitting physicians to prescribe antidote drugs like Narcan.
Narcan now costs $25 to $40 per dose, and it's currently available for over-the-counter sales in CVS stores in 14 states without a prescription. Recovery specialists like Cicchino are contacted by the hospitals participating in Barnabas' program once a Narcan call has been dispatched, with the aim of immediately getting individuals into recovery and rehabilitation programs.
"That's why this program is so special - the empathy we bring, we represent the hope that they can get out of the addiction," said Cicchino, who grew up in Ocean County and was for years addicted to painkillers, as well as alcohol and other drugs.
Since she began working with the program when it launched three months ago, there have been 135 overdoses in Ocean and Monmouth counties, of which 30 were fatal. The Ocean County Prosecutors Office told CBS News that, thanks to this new recovery program, and the input of recovering addicts, about 50 percent of those revived with Narcan agreed to go into treatment since January- compared to a prior success rate of "virtually zero."
Medical communities and the opioid epidemic
As part of the broader U.S. government response to the opioid epidemic, the CDC last March also issued new guidelines, specifically to doctors, on prescribing opioid painkillers for chronic pain, including opting for non-opioid painkillers as a first choice except where a person is being treated for cancer, and prescribing the lowest dose possible to effect pain relief.
"I don't think that painkillers are awful," said Cicchino. "Somebody who's going through chemotherapy or on their deathbed, I'm not saying they shouldn't be on some kind of pain medication [but] to the 17-year-old who broke their leg at a soccer game, and they're getting prescribed (80-milligram Oxycodone tablets), I think it's a problem. I think that there needs to be more structure to how it's prescribed."
In New York, Ruiz, the retired bus driver, echoed that sentiment.
"I'm hoping that the medical field can come up with something that's not addictive that can help me," said Ruiz, as he browsed through old photo albums, picking out his favorite photographs, of his family, of his days as an amateur hockey player. His youngest daughter, enrolled in middle school, sat beside him.
"I want to push out (painkillers) and I want to stay off," said Ruiz. "I want to have some kind of life without this stuff."