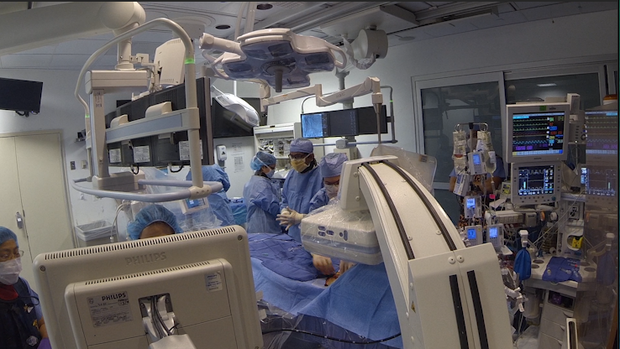
A life-saving alternative to open heart surgery
Dr. Susheel Kodali kept his gaze fixed on the four monitors suspended above the patient he was operating on at NewYork-Presbyterian/Columbia University Medical Center's Heart Valve Center.
"You see, one of the keys to this procedure is imaging, because we're not opening the chest, so we use all modalities available including X-Ray and echo," he said.
Kodali and his team have performed more than 1,200 transcatheter aortic valve replacement (TAVR) procedures just like this one, more than any other institution in the U.S., since TAVR was approved by the FDA three years ago. It's a non-invasive alternative to heart surgery that replaces the aortic valve, responsible for pumping blood out of the heart, via a narrow tube called a catheter. The catheter is expanded using a balloon structure, much like a heart stent, and through it a replacement valve is fitted into place.
Because TAVR does not stop the heart or require putting the patient on a heart-lung bypass machine, it's made treatment for aortic valve conditions accessible to thousands of patients, mostly elderly, who would otherwise have been deemed "too risky" for open heart surgery and left with no other options. And compared to open heart surgery, the recovery period after TAVR is much less difficult.
With ongoing advances in technique and technologies, specialists like Kodali say TAVR will soon present an alternative to traditional surgery for most patients, not just the ones who currently meet the required criteria.
"Surgery is great but it's not improving, for the most part they've perfected what they can do," said Kodali. "But now, with TAVR, we're just at the infancy, it's within 10 years and such a rapid rate of iteration... I think we'll be doing it in a large majority of patients that need valve replacement."
For now, however, TAVR is not recommended for younger patients because its long-term durability is unproven.
The first TAVR procedure was done in France 12 years ago. Doctors began clinical trials in the U.S. in 2005, led by the director of the NewYork-Presbyterian/ Columbia University Center for Interventional Vascular Therapy, Dr. Martin Leon.
"Aortic stenosis is the most common disease of aging in heart valve patients," Leon told CBS News. "Before TAVR, 30 to 50 percent of them were literally left behind, with no therapy, with a rapid downhill course. That was the basis of developing this newer, less invasive technique."
Aortic stenosis, the narrowing of the aortic valve opening, occurs in roughly 5 percent of all people over the age of 75. In America it affects 300,000 people, and many require a heart valve replacement. Left untreated, severe symptomatic aortic stenosis carries a poor prognosis; up to 60 percent of patients will die within 2 years, and fewer than 30 percent will survive 3 years.
Leon explained that that TAVR does not extract the old, failing valve, but simply displaces it within the heart and replaces it with a new valve.
"We've developed techniques that minimize the likelihood of problems arising from the old valve remaining in the heart," said Leon, adding that the shrinking size of catheters and types of transcatheter valves used are also improving even faster than many experts expected.
Two types of replacement transcatheter valves are currently on the market in the U.S.: the Edwards SAPIEN and the CoreValve system. The former requires a balloon structure to inflate the valve once in the heart, while the newer CoreValve system is self-expanding.
"The low rates of stroke and valve leakage with the CoreValve System - two of the most concerning complications of valve replacement because they increase the risk of death and have a dramatic impact on quality of life - set a new standard for transcatheter valves," said Jeffrey J. Popma, co-principal investigator of the most recent transcatheter valve trial.
TAVR is done in an operating room set up to easily convert to a full surgery in case complications arise, and it involves a collaboration between various medical specialists.
"There will always be an interventional cardiologist, a surgeon, an imaging expert, all in the same room sharing their skills in order to take care of these very difficult patients," said Leon.
Mary Fuller, 67, was one such patient of Kodali's earlier this year. She had already had open heart surgery six years ago. When she found out that she needed another valve replacement, but was too sick to undergo surgery again, she thought she was out of options.
"I thought, I was lucky enough to have lived this long, and I thought maybe I'm pushing my luck," said Fuller.
When she heard about TAVR, she immediately signed up, and says she's had no regrets.
"It was quite a remarkable thing and I would recommend anyone to just go for it and not be afraid. I had the most wonderful doctors and nurses reassuring me every step of the way," said Fuller, who was quickly back to her job as a psychology professor following surgery. "The most amazing thing is, I was home within three days!"
According to Kodali, patients sometimes leave the hospital the day after their procedure. "It's relatively painless," he said. "They're awake during catheterization, and some of the patients we operate on are awake during the procedure."
As yet, TAVR is offered by only a handful of hospitals in the U.S. However, doctors say that as it improves it should become increasingly accessible to more people.
"Most of the patients I treat are going for a treatment for quality of life," said Kodali. "Most of them say I don't care if I will long but I can't live like this."
"I think the devices and procedures are going to look very different in 10 years and our patients will benefit enormously from it," he added.
According to Fuller, her quality of life after TAVR is already an improvement compared to traditional surgery, which had taken her months to recover from: "I can't say I'm bouncing around, but I'll tell you I was running from my classroom to my office and people literally had to run to keep up with me."
Eliene Augenbraun contributed reporting.