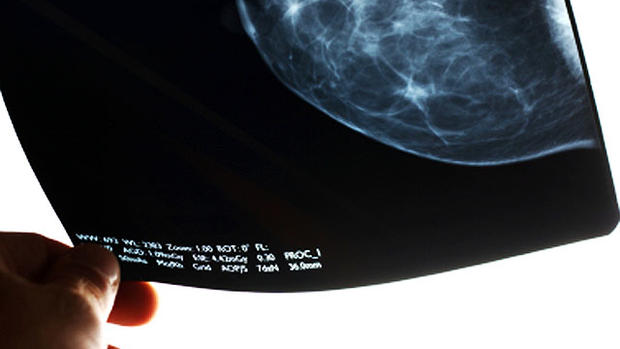
Study: Mammogram benefits outweigh risks for some women in their 40s
(CBS News) Routine mammograms have both benefits and potential harms for women in their forties. A new study weighs the two consequences - and finds that for certain women between the ages of 40 to 49 with risk factors for breast cancer, the benefits outweigh the potential harms.
Busted! 8 mammogram truths every woman must know
Mammograms may lead to breast cancer "overdiagnosis" for some women
Mammograms save fewer lives than many think, study shows
The study, published in the May 1 issue of the Annals of Internal Medicine, looked at data from three national research groups: the Breast Cancer Surveillance Consortium (BCSC), Cancer Intervention and Surveillance Modeling Network (CISNET) and the Oregon Evidence-based Practice Center.
Benefits of mammography exams include gaining years of life and preventing breast cancer deaths. Harms include false-positive exams that may lead to unnecessary biopsies or surgeries, pain and anxiety.
The main finding from the new study was women with certain risk factors that amount to a two-fold risk of developing breast cancer would benefit from mammogram screening every other year. According to the researchers, women who are at a higher risk for breast cancer include those with
extremely dense breasts (13 percent of the population ages 40 to 49) or
having a first degree relative with breast cancer (9 percent of the same
population).
"Our research suggests the benefit-harm balance is tipped in favor of every-other-year screening for women in their 40s who are at about twice the average risk of developing breast cancer," Dr. Jeanne Mandelblatt, study author and associate director for population sciences at Georgetown Lombardi Comprehensive Cancer Center, said in a written statement. "The study also determined that the balance of benefits and potential harms in this same group is not favorable when increasing the frequency of mammography screening to once a year."
The study also compared digital mammography with film mammography and found greater harms from digital screenings - digital exams were more likely to result in false positives.
The risk factors identified by the study might change screening guidelines for women, but Mandelblatt emphasizes they should not be taken as individual recommendations for a person. Such guideline changes might include trying to determine a woman's breast density, she said.
"For example, the need to have a mammogram to determine breast density is an important point to consider in regards to implementing risk-based guidelines based on breast density," Mandelblatt said, adding that some groups might see this as a reason to recommend a baseline mammogram for women.
"Ultimately, though, the decision of when to start screening and how often, and whether to have digital or film mammography should be left to women and their health care providers," she said.
The National Cancer Institute has more on mammograms.