Like Instagram for doctors, with many second opinions
Dr. Alan MacGill, a foot and ankle specialist in Boynton Beach, Florida, sees many complicated cases at his private practice. MacGill sometimes wishes he could get a second opinion from a colleague before making any critical decisions about a patient's care.
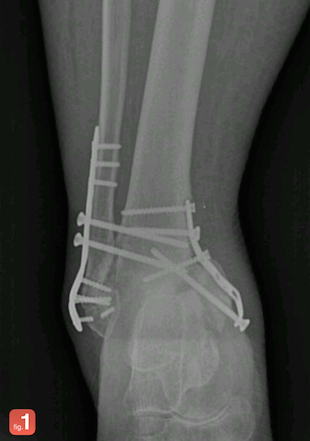
One recent case stands out in his mind. A 64-year-old woman had a prior ankle fracture repaired some time ago by another doctor using extensive hardware. The fracture had now deteriorated, and as a result her joint had collapsed and the hardware broke. She also had a history of diabetes, obesity, poor circulation in the limbs and multiple blocked blood vessels in her leg.
"It was a really difficult situation because when that happens that has to be revised and the chances of failure are really high," MacGill told CBS News. "And those patients are really at risk for losing their leg."
MacGill wasn't sure if he could salvage his patient's ankle and he wanted to check his gut instinct on what he should do.
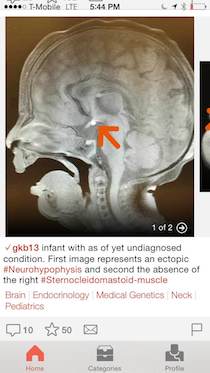
So he posted X-ray images and a description of the case on Figure 1, a phone app that allows physicians, medical students, nurses, emergency medical technicians and other health care professionals to share images and case studies of patients for educational purposes.
It didn't take long until there were 19 comments from foot and ankle specialists, orthopedists and others familiar with the this type of case. They were communicating amongst each other with MacGill about whether the ankle could be salvaged.
"Did you consider trying to reduce it?"
"Did you consider using a plate?"
"Did you consider using an arthroscopic fusion?"
"Tough call, you can always do BKA [below-knee amputation] later if initial surgery fail."
MacGill says the exchange over the app helped reinforce his gut instincts for how to treat his patient.
"We were able to kind of take a good approach for her and really optimize her before that surgery," he said. "Fortunately it healed and she is doing very well now. And that really helped make the difference between whether we're choosing amputation as an option versus trying to save the limb with a really complex surgical procedure."
Figure 1, a sort of Instagram for the medical set, is one of the many digital tools helping to shape the way doctors communicate, develop their skills and deepen their understanding of medicine. Launched in May 2013, the app currently has more than 150,000 users in the medical field worldwide.
Dr. Joshua Landy, Figure 1's co-founder and an internal medicine and critical care specialist based in Toronto, Canada, said he had always wanted a way to connect with colleagues about his patients when he couldn't "do it justice with words."
"I wasn't the only one who faced that struggle with the efficient transmission of information," Landy told CBS News. "That's something that every emergency doctor knows about, every family doctor knows about."
Landy then became interested in understanding how clinicians share information and advice. He landed a fellowship at Stanford to research a simple but fundamental question in this mobile tech-obsessed culture: "What do young physicians and med students do with their smartphones at work?"
"And what we found was some very unsurprising things like they used it to call each other and text each other," said Landy. "But those behaviors were also mixed with the sort of unstructured education behaviors, which would be the type of informal learning that you get just by talking about cases with other colleagues at work."
A few years later, the app is servicing millions of images each day from all over the world.
Information sharing has become increasingly more important in the medical profession, especially as hospitals and medical institutions go digital. Even the government's Center for Medicare and Medicaid Services is catching up with the times by now covering remote doctor visits through their telemedicine service.
SERMOS, an online social network launched in 2005, connects doctors in the U.S. and plans to expand to the U.K. The website has a following of more than 340,000 members who also share case studies and seek advice from other users to help diagnose and treat patients. In a survey conducted by the company, 75 percent of U.S. doctors said at least 20 percent of patient cases fell in the grey zone and required input from other colleagues.
Landy says in developing the app his company has made extensive efforts to remain compliant with patient privacy protections such as the Health Insurance Portability and Accountability Act (HIPAA) in the U.S. and similar laws throughout the world. These regulations provide specific instruction on what can and cannot appear in photos, such as faces and tattoos. The app provides tools such as an automatic face-blocking feature that detects faces and blocks them, helping users adhere to the laws. Other features include an in-app "tap, type, and sign" consent form for clinicians practicing in countries or medical facilities that require written patient consent for photos.
MacGill sees this as critically important. "I've had some friends in the medical profession who had posted on Facebook and I always thought that wasn't really the appropriate place for it because of either privacy violation or maybe because the other people in that community didn't necessarily want to see that," he said.
MacGill says Figure 1 provides a forum for physicians to become familiar with cases they'd probably never see face-to-face. "It kind of opens up your world and opens up your eyes to just the other aspects of medicine. From the first day I immediately became hooked," he said. "I think that medicine is so specialized now that at the end of our training we kind of are confined to our little box, and sometimes we only see what we see through our little blinders."
This information is valuable in a world where many illnesses once thought rare or exotic are now merely a plane ride away. Some users of the app are doctors working overseas who want advice on how to help their patients with severely limited resources.
Landy said recently there were two medical students working at a facility in the Solomon Islands who had a patient they suspected was having a heart attack. They had on-hand only an out-of-date electro-cardiogram machine and some expired medication. The students posted details of their predicament, and others on the app offered their recommendations.
"Having people weigh in and having people give you a bit of guidance, or I suppose reaffirm what you suspect, is valuable," said Landy. "It's like having a colleague, or having many, in your pocket to bounce ideas off any day or night."