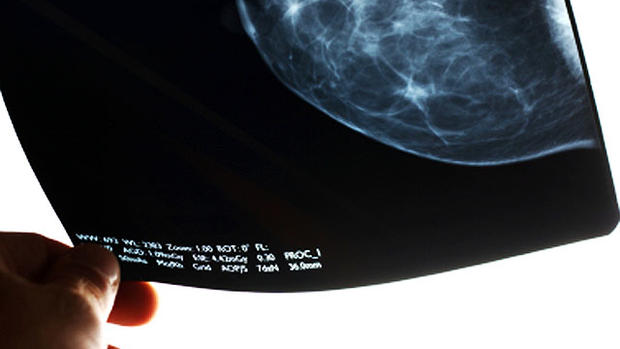
Breast cancer studies spotlight "false positive" mammograms, digital scans
(CBS) Mammography can save live by finding breast tumors early, when effective treatment is still possible. But by leading women and their doctors to believe that a perfectly healthy breast is cancerous, a "false positive" mammogram can cause needless anxiety as well as needless - and risky - follow-up care.
PICTURES - Busted! 8 mammogram myths every woman must know
Just how common are false positives? To find out, researchers studied almost 170,000 women who had their first screening mammogram in their forties or fifties and about 4,500 women who had been diagnosed with breast cancer.
The researchers found that more than half of women who start getting annual mammograms in their forties can expect to have a false positive, being called back in for additional screening. Of the women who are called back, about 7 percent are advised to undergo a biopsy of the breast that turns out to be negative (meaning no cancer is present).
Screening every other year rather than annually can cut the risk of getting a false positive by about a third, the researchers found. But biennial screening was tied to a slight increase the risk that a tumor would be missed until it became advanced.
So it's a trade-off: more false positives with annual screening vs. fewer false positives with increased risk for being diagnosed with late-stage cancer. But the researchers concluded that "mammography every year is less efficient than screening every two years or more."
No matter what screening regimen women decide upon, it may be helpful to know that false positives are so common.
"We hope that by helping women know what to expect in terms of false-positive results, they'll be less likely to experience anxiety when they are called back for a repeat screening or biopsy," study author Dr. Rebecca Hubbard, assistant investigator at Seattle's Group Health Center for Health Studies, said in a written statement.
In a related study, researchers studied more than 300,000 women who had undergone mammography between 2000 and 2006 to gauge the accuracy of two popular mammography screening technologies - traditional film mammography versus digital mammography, which is increasingly popular. The researchers found that for most women, the two screening techniques have about the same accuracy.
However, digital mammography was found to be more accurate at detecting so-called estrogen receptor-negative cancer in extremely dense breasts. Since dense breasts and estrogen receptor-negative tumors are more common in younger women, the study authors concluded that digital may be better for women 50 to 79 years of age.
The studies were published in the Oct. 18 issue of Annals of Internal Medicine.
Experts disagree on how frequently women should undergo mammography, and at what age they should begin. The U.S. Preventive Services Task Force triggered a firestorm of controversy in 2009, when it suggested that the decision about whether to start mammography before age 50 should be based upon a variety of factors, including the patient's risk level. The American Cancer Society continues to recommend annual mammography screening for all women starting at 40.
The National Cancer Institute has more on mammography.